Psoriasis, skin disease
Written by:Psoriasis is an inflammatory disease that affects the skin and sometimes the joints. It is a chronic pathology that occurs in outbreaks, that is, with periods in which the lesions and associated symptoms appear or worsen, and other periods in which they refer or improve. It is a condition with a wide range of severity , from mild to moderate and severe. It is important to emphasize that psoriasis is not contagious and, therefore, the people who suffer it do not transmit it to others with whom they have contact.
Is it a common pathology? How does psoriasis affect those who suffer?
Around 3% of the population have psoriasis. In Spain, it is estimated that more than one million people suffer from this disease.
Psoriasis affects all areas of life of the person who suffers : physical, psychological and emotional, social and work. This involvement is usually greater in people with moderate to severe psoriasis than in people with mild psoriasis, but severity is not the only factor to be taken into account since other influences such as: location of lesions, age, personality, profession, etc.
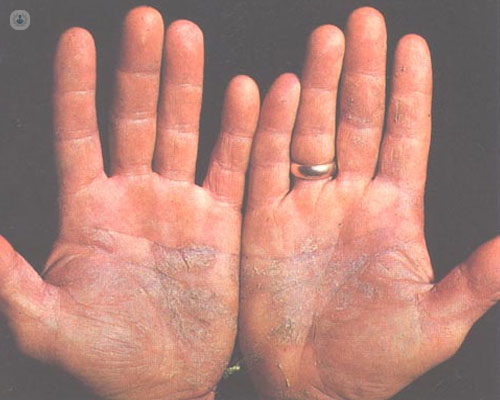
Symptomatology of psoriasis
Its most common clinical manifestation is the appearance of lesions on the skin in the form of plaques of variable size, red and with whitish scales on the surface. It can also affect the nails of hands and feet appearing thickening, detachment of the final part, yellow spots, small dimples, among others. If it affects the joints , it is what is called psoriatic arthritis, inflammation and pain of one or more joints (very typically the joints of the fingers), pain in the heel or appearance of inflammation in a finger (which takes on the appearance of a sausage).
Causes of psoriasis
From a physiological point of view psoriasis consists of the abnormal proliferation of skin cells. In a normal situation the skin regenerates in about 30 days, but in psoriasis it does so in just 4 days. This causes the skin cells to accumulate and form plaques with scales characteristic of the disease.
Psoriasis is caused by a combination of genetic and environmental factors. There is a genetic component that predisposes to psoriasis and it is estimated that about one-third of affected patients have direct relatives with psoriasis. In addition, there are triggers or precipitants that cause the outbreak to appear: stress, alcohol, obesity, certain medications, infections, hormonal changes ...
Psoriasis: Treatment
Each person with psoriasis has particularities that have to be taken into account when choosing a treatment or another: severity and type of psoriasis, location of the lesions, other concomitant diseases, sex, age, profession, lifestyle, degree of affectation Psychological, repercussion on the quality of life, personal preferences ... There are treatments that work in some patients, but they do not work or even go wrong in others. For this reason, the treatment must be personalized for each patient. I usually expose and explain to my patient the different options for together to be able to decide the most appropriate therapy in your case.
And what therapeutic options are there at the moment? We can divide them into four main groups :
- Topical treatments are creams, ointments, lotions, foams or shampoos containing various active ingredients (corticosteroids, vitamin D derivatives, retinoids, calcineurin inhibitors) that are applied to affected areas. They are usually suitable treatments for mild cases or localized lesions.
- Phototherapy : therapy with ultraviolet light type A or B (UVA or UVB) that are emitted in cabins under medical supervision. A natural version of phototherapy consists of sunbathing in a controlled manner.
- Systemic treatments (cyclosporine, methotrexate, acitretino): are treatments in pills or injections that act in the organism of global way. They are more effective than topical treatments but can also have more side effects that need to be taken into account and properly controlled.
- Biological treatments and small molecules (etanercept, adalimumab, infliximab, ustekinumab, ixekizumab, secukinumab, apremilast): this is the latest generation of treatments for psoriasis. They are the most effective and are indicated for moderate or severe cases that have not responded or have had side effects with previous treatments. They are very expensive drugs that are obtained in the pharmacy of the hospital under medical prescription. Biological drugs are all administered with a syringe or pen (insulin-like) injection, except for infliximab which is given by intravenous infusion in the hospital. The apremilast, which is considered as a small molecule, is a pill that is taken twice a day. It is not as effective as biological treatments, but it is very safe, it can be effective in certain difficult-to-treat locations (palms and plants, scalp) and controls itching very quickly.
What progress has been made in recent years in the treatment of psoriasis? What does it consist on?
In recent years, thanks to the research of the pharmaceutical industry along with the efforts of the medical community and the inestimable predisposition of patient support, there has been great progress in the treatment of psoriasis. I myself have had the opportunity to participate in several clinical trials in this field. The appearance of biological drugs and small molecules has been a new scenario in the treatment of psoriasis because of its efficacy and safety clearly superior to what until that moment we handled.
We currently have six biological drugs marketed and new. In addition, there has recently been another important advance with the commercialization of a new topical spraying treatment in foam , novel in its efficacy, which is superior to the rest of topical treatments, and for its ease of application, since at It is a foam that spreads very well and is not so tacky. These advances give us dermatologists very useful tools to help our patients to control psoriasis and improve their quality of life .
For more information on psoriasis, consult with a specialist in Dermatology .



