Psoriasis Types and Treatments
Written by:In my previous article I explained what is psoriasis, its causes and epidemiology , so now I expose the types and treatments of this disease that suffer more than 125 million people worldwide.
The clinical manifestations of psoriasis are very varied but the most frequent is psoriasis vulgaris or plaque characterized by the presence of well-defined symmetric erythematoscamous plaques of preferential localization in extensor zone of extremities and in leather. The lesions are usually asymptomatic although patients usually report itching. Other clinical forms are:
- The guttate psoriasis that mainly affects children and adolescents, presents with plates of 2-5 mm in diameter that usually appear on the trunk and extremities.. They usually appear abruptly after a throat infection.
- Inverse or inverted psoriasis, also known as flexural psoriasis, predominantly affects the inguinal, anal and axillary folds and the lateral aspect of the neck.
- Pustular psoriasis is a rare form of the disease, in which multiple sterile pustules of approximately 2 to 5 mm are seen on an erythematous basis and often occur as a result of irritation from topical, systemic or even after treatment. of the suppression of systemic corticosteroids.
- Erythrodermic psoriasis is the least frequent form and is characterized by extensive redness that affects up to 50% of the skin surface.
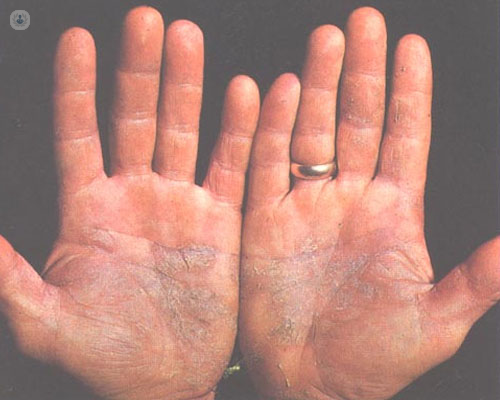
Joint and nail involvement of psoriasis
The involvement of the nails in psoriasis varies between 13% and 50% of affected people and their frequency increases when the disease starts before the age of 30, is accompanied by arthritis (where it reaches 70%) or reaches a serious gravity.
Regarding joint involvement in psoriasis, its incidence ranges very widely between 1 and 42%, which is undoubtedly influenced by the different criteria used for its definition and by the specialist who treats it. Arthritis is more frequent among those patients with nail involvement or who suffer from erythrodermic and pustular psoriasis. Psoriatic arthritis is a special type of asymmetric seronegative inflammatory arthritis that most commonly affects the distal periarticular joints and structures of the fingers and toes as well as the spine.
Treatment for psoriasis
In the absence of a curative treatment , the goal of treatments for psoriasis is to rid the skin of lesions for as long as possible : this is what is called "cleaning" or "clearing" the plaques of psoriasis. There are many treatments for psoriasis, the choice of one or the other will depend on the type and severity of the psoriasis (measured by indexes of extension and severity -PASI, BSA, PGA- and quality of life), location of the lesions, age and sex of the patient and of the individual characteristics (concomitant pathologies and habitual medication, etc).
There are topical treatments (corticosteroids, retinoids, vitamin D derivatives, ...), phototherapy (PUVA, UVB, laser therapy with excimer) and systemic treatments (cyclosporine, methotrexate, acitretin, esters of fumaric acid, hydroxyurea). These systemic treatments, used in moderate or severe psoriasis , are associated with potential serious side effects, especially in prolonged treatments. Therefore, cyclic, rotational and sequential therapy is used to reduce the risk associated with these systemic medications.
New drugs for psoriasis
In recent years the emergence of new drugs generated by molecular biology using recombinant DNA technology and directed against cytokines or surface proteins of lymphocytes blocking specific steps of the pathogenesis of psoriasis (biological therapy) has been a revolution in the treatment of psoriasis. These drugs have demonstrated high efficacy allowing long-term control of the disease in monotherapy.. There are more than 40 molecules analyzed for the treatment of psoriasis. The currently approved drugs for the treatment of moderate-severe psoriasis are etanercept, infliximab, adalimumab and golimumab (anti-TNF drugs). Anti IL12 / 23 drugs: ustekinumab.
All these biological treatments seem relatively safe in the short and medium term and have not been shown to be hepatotoxic or nephrotoxic or show drug interactions (unlike conventional systemic therapy). However, the risk of long-term immunosuppression and of developing infections or neoplastic processes should be monitored.. Special attention to the development of infections such as tuberculosis should be followed fundamentally with the use of anti-TNF.
Undoubtedly, the new biological therapy is assuming a revolution in the management of the psoriatic patient , allowing an effective medium-long term control of the disease. New advances in pharmacogenomics in addition will probably allow in the future to individualize this biological therapy in each patient choosing the most effective and safe drug in each case. In the coming years, drugs such as Apremilast, tofacitinib, and anti-IL-17 antibodies will appear to control patients with psoriasis.


