The Gleason score for prostate cancer
Written by:The Gleason score has its origins in 1977, when its creator Donald Gleason developed the model to classify prostate cancer. It has undergone modifications that have been aimed at homogenizing the interpretation of prostate biopsies, so that the Gleason score of a European pathologist is equivalent to the score of one American.
What is the Gleason score for prostate cancer?
As reported by specialists in urology, when a prostate biopsy is performed, a representative number of punctures are collected from the gland. Each punch draws a cylinder one millimeter in diameter by 15 in length. Usually extracted from 12 to 24 cylinders that are sent to the Department of Pathology, where the samples are processed with alcohols and paraffins as well as dyes. They are then deposited in a glass for the pathologist to examine them under the microscope and give their verdict.
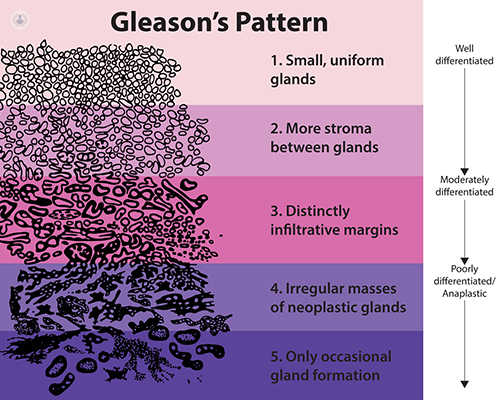
Gleason score for prostate cancer
When the pathologist confirms that there is cancer the next step is to specify the Gleason score consisting of two numbers, a primary grade and a secondary grade. The primary grade determines which type of tumor predominates and the secondary degree specifies the maximum aggressiveness that it has observed. Numbers 3 to 5 are used.
- If the tumor tissue is not aggressive, it will be scored with a 3
- If the tumor tissue is extremely aggressive it is assigned a grade of 5
- Score 4 is reserved for intermediate aggressions
Primary and secondary numbers are added together to create a Gleason score ranging from 2 to 10. Some examples are:
- Gleason 3 + 3: this is a patient who has a biopsy in which has been observed a very aggressive cancer, in addition all the cancer cells have equal aggressiveness.
- Gleason 3 + 4: this case is a cancer where the cells have been objectively aggressive with other cells of intermediate aggressiveness, but the cells are less aggressive.
- Gleason 4 + 3: type of cancer where non-aggressive cells have been objectified with other cells of intermediate aggressiveness. However, cells of intermediate aggressiveness predominate over the less aggressive ones.
- The worst score will be 5 + 5 or what is the same, this patient has a very aggressive prostate cancer and all the cells are very aggressive.
Gleason score is a prognostic variable. Of course, tumors with Gleason scores 5 + 5, 5 + 4, 4 + 5 are tumors that are very aggressive and perform worse than those 3 + 3 or 3 + 4. Men with low-grade prostate cancer are often monitored with active surveillance and have frequent screenings that may include PSA tests, digital rectal exams, ultrasound, or other imaging along with repeated biopsies.
The most common Gleason score
A 5-7 or G2 score is considered intermediate or has moderately differentiated cells. Most prostate cancers fall into this category, making it difficult to predict their development. This tumor is found between an early stage and a more aggressive stage. Again, it usually means that the cancer is unlikely to grow or spread for many years, but a doctor may recommend treatment such as surgery or radiation depending on the patient's age and overall health. If it is treated during this intermediate stage, it gives a man the best possible result and can extend years into his life.
The worst prognosis for a patient with prostate cancer
An 8-10 or G3 score is considered high grade with poorly differentiated cells. This means that the tumor is at an advanced stage and the cancer is considered high risk. If the cancer has not spread beyond the prostate gland, it is still possible to treat it successfully, which is usually done with surgery. Sometimes radiation is needed after surgery if the prostate cancer cells have been found beyond the prostate gland.


