The sacroiliac pain: the great unknown
Written by: 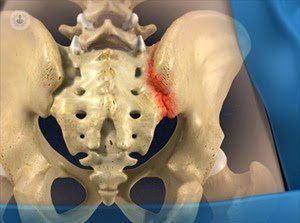 The sacroiliac joint (ASI) is responsible for 15-25% of cases of chronic low back pain. The difficulty for diagnosis makes sacroiliac pain is often undervalued and not treated properly, resulting in chronic pain conditions in long-term evolution. Many patients with unilateral low back pain, pain radiating to leg or hip or gluteal region actually suffer pain of ASI. The complex anatomy of this joint may be responsible for their ignorance and diagnostic difficulties.
The sacroiliac joint (ASI) is responsible for 15-25% of cases of chronic low back pain. The difficulty for diagnosis makes sacroiliac pain is often undervalued and not treated properly, resulting in chronic pain conditions in long-term evolution. Many patients with unilateral low back pain, pain radiating to leg or hip or gluteal region actually suffer pain of ASI. The complex anatomy of this joint may be responsible for their ignorance and diagnostic difficulties.
Fortunately, each time more specialists in Pain Unit will increasing awareness of the existence of this table and are improving the criteria for proper diagnosis and treatment.
Location of pain in the sacroiliac joint
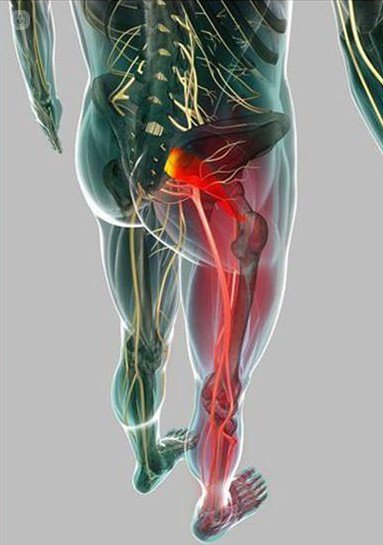 The sacroiliac joint pain often associated with pain from the lower lumbar vertebrae. Typically it reflected as low back pain (75%), pain in gluteal area (94%) or pain radiating to the leg (28%). The pain may originate in any of the structures of the sacroiliac joint: articular surfaces, periarticular sacroiliac ligaments and muscles, or a combination thereof.
The sacroiliac joint pain often associated with pain from the lower lumbar vertebrae. Typically it reflected as low back pain (75%), pain in gluteal area (94%) or pain radiating to the leg (28%). The pain may originate in any of the structures of the sacroiliac joint: articular surfaces, periarticular sacroiliac ligaments and muscles, or a combination thereof.
Diagnosis of pain in the sacroiliac joint
The clinical diagnosis by screening and provocation tests can be very unclear. No clinical trials that reference a symptom with a specific disease. Most indicative is whether unilateral pain below the L5 vertebra or palpation of the ASI and the absence of other diseases such as tumors, tumor or inflammation or neurogenic pain. Also conventional radiology, ultrasound and MRI may result in a high number of false positives and negatives, so it is considered the best diagnostic method is a test block of the sacroiliac joint with local anesthetic. It is a simple lock that is performed under radiologic or ultrasound scan and if positive confirms the diagnosis and establishes the basis for definitive treatment.
Treatment of pain in the sacroiliac joint
Conservative treatments such as anti-inflammatory drugs and analgesics, rehabilitation and physical therapy, intra-articular injections of steroids, etc. have proved effective only in some cases, but still must be pre-tested in more aggressive actions.
 In resistant cases, the therapy of choice is the RF nerve fibers reaching the sacroiliac structures, ie, in the back L5 and S1 branch, S2 and S3. The scope of the nerves to the ASI is mostly dependent on subsequent branches, making them accessible to the posterior approach with limited risk. The variability of the results by the anatomical differences explained in the distribution of innervation sacroiliac. In any case it is a procedure performed on an outpatient basis but within the sterile environment of an operating room. It is interrupted by current carrying the fibers painful and innervation of ASI is done percutaneously.
In resistant cases, the therapy of choice is the RF nerve fibers reaching the sacroiliac structures, ie, in the back L5 and S1 branch, S2 and S3. The scope of the nerves to the ASI is mostly dependent on subsequent branches, making them accessible to the posterior approach with limited risk. The variability of the results by the anatomical differences explained in the distribution of innervation sacroiliac. In any case it is a procedure performed on an outpatient basis but within the sterile environment of an operating room. It is interrupted by current carrying the fibers painful and innervation of ASI is done percutaneously.
 Among the many methods used radio frequency and widely studied, improvements are reported in 50-70% of patients for such a long time as 36 months. intraarticular fixed radiofrequency is less effective (50%), the "cold" RF causes lesions larger but their effectiveness has not been shown greater. Among the methods I prefer for its more effective include the so-called method of the palisade (consisting of placing the electrodes at a distance of 6 cm from the sacral foramina into the joint, forming a continuous line of interruption of nerve traffic (image left)) or the most difficult technically, the selective blockade of the dorsal roots L5 and S1, S2 and S3 to the output of the sacral holes (right image) using bipolar radiofrequency.
Among the many methods used radio frequency and widely studied, improvements are reported in 50-70% of patients for such a long time as 36 months. intraarticular fixed radiofrequency is less effective (50%), the "cold" RF causes lesions larger but their effectiveness has not been shown greater. Among the methods I prefer for its more effective include the so-called method of the palisade (consisting of placing the electrodes at a distance of 6 cm from the sacral foramina into the joint, forming a continuous line of interruption of nerve traffic (image left)) or the most difficult technically, the selective blockade of the dorsal roots L5 and S1, S2 and S3 to the output of the sacral holes (right image) using bipolar radiofrequency.
These techniques performed with appropriate precautions, checking sensory and motor reaction and impedance (ratio between applied voltage and current and the response produced in the body), only reported side effects and can be performed with mild sedation in 20-40 minutes, It is on an outpatient basis.
Edited by Roser Berner Ubasos


