Do you know the risks of amniocentesis?
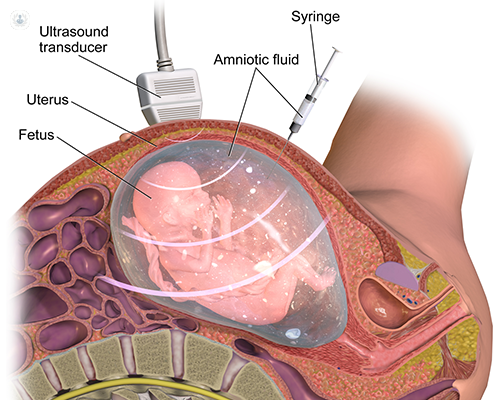
Written by:Amniocentesis is an invasive procedure that involves inserting a thin needle through the mother 's abdominal wall to aspirate a sample of amniotic fluid. This sample allows to study various features of the fetus and pregnancy.
The patient does not require any special preparation, not even be fasting, they will only verify a number of analytical parameters such as blood type or serology.
The main application today amniocentesis is the study of fetal chromosomes. For example, when you have performed a screening of chromosomal abnormalities with high-risk result and a confirmation is required with the study of chromosomes. Specialists in Gynecology also recommend to do it in situations of suspected fetal infection, known as corioamnnionitis.
When to perform an amniocentesis?
Amniocentesis is a test that is given from the 16th week of pregnancy onwards, ie, after 4 months of gestation. Once this period can be performed at any time during pregnancy; whenever it deems appropriate for the study of the fetus.
Amniocentesis risks
The main risk of amniocentesis is fetal loss. The risk exists is close to 0.50% in the hands of an experienced operator. There is also a small risk, estimated at 0.30% of premature rupture of membranes or amniotic fluid infection. There are other risks as very rare placental bleeding, hematoma of the abdominal wall or fetal trauma.
Alternative techniques to amniocentesis
Amniocentesis is currently being replaced, in some cases, by the genetic test noninvasive maternal blood. This test is performed as evidence for the study of chromosomes of the fetus by the absence of complications or risk to the fetus supposed to be tests called NIPT. However, amniocentesis still has its place as evidence for definitive study of alterations of chromosomes and study of fetal infections.



