ultramínimamente ecoguide invasive surgery tarsal tunnel syndrome, an under-diagnosed problem
Written by:Tarsal tunnel syndrome is a compression neuropathy of the posterior tibial nerve or one of its branches, when it passes below the flexor retinaculum (lacinado ligament) and / or below the adductor muscle of the first finger.
Clinic tarsal tunnel
Patients have heel pain, irradiated or not the lateral side thereof or to the forefoot. They may be associated burning sensation, cramps, numbness or other paresthesias. Patients often experience relief when taking off your shoes and socks or stop walking.
The pain can be at rest but can severely limit ambulation of patients unable to walk moderate or small distances or sports.
If we accept that 10% of the population (compared to 3-5% with the syndrome carpal tunnel) will have heel pain throughout their lives and that many of these cases are not fasciosis plant, but peripheral neuropathies, Perhaps this is the most common peripheral neuropathy.
In many cases we see that patients take years to 20 years, with heel pain plantar falsely treated as fasciosis without any improvement.
Causes of tarsal tunnel syndrome
While 20-40% of cases do not get to determine the cause, most often we found in the posterior tibial nerve compression or one of its branches in the tarsal canal.
The most common causes of tarsal tunnel syndrome are space-occupying lesions (traumatic, neoplastic or inflammatory). These include varicose veins (which are the most common), tenosynovitis, or ganglion cysts and neurilenomas. Less common are the lipomas, neurofibromas and malignant tumors.
If we focus on posttraumatic factors, they account for 20% of cases. Examples include ankle fractures, sprains and dislocations or fractures of the calcaneus or, more rarely, nonunion of sustentaculum tali (if migrates superiorly into the tunnel can cause posterior tibial nerve compression). Also they fall within this group bone abnormalities, including tarsal coalition, which have been described as causes of this syndrome.
On the other hand, this syndrome has been associated with systemic diseases such as diabetes and rheumatoid arthritis, hypothyroidism, hyperlipidemia and seronegative arthropathies. Other less common causes include muscle hypertrophy abductor hallucis, the flexor of the fingers or the existence of accessory muscles.
In addition, recent studies show that certain deformities such as flat feet or a fixed hindfoot valgus, increase the tension on the posterior tibial nerve.
It may also be involved in the development of tarsal tunnel syndrome varus deformity of the heel with a secondary foot pronation.
Diagnosis of tarsal tunnel syndrome
To diagnose the syndrome tarsal tunnel most important is the clinical history and examination. L electromyography is negative in most cases, so that this entity is underdiagnosed.
The ankle and foot radiographs allow us to evaluate the structure of the foot (flat foot, foot I dig), the existence of fractures, bone mass, bone spurs and coalitions of the subtalar joint. Laboratory studies detect metabolic or rheumatic problems.
Furthermore, Perthes test (with a tourniquet compression) causes an occlusion of the superficial venous system; if the deep system is incompetent, the posterior tibial vein is completed and reproduce the symptoms.
Meanwhile, the EMG can examine the latency, amplitude and velocity of the posterior tibial nerve and its accompanying branches, while the QST techniques quantify the perception of pressure and vibration.
MRI should be performed to rule out any bone or soft tissue injuries that result in a compression of the NTP.
It will make the differential diagnosis with L5 or S1 radiculopathy, or a sensory polyneuropathy (this is bilateral and has distribution sock and Tinel).
Treatment of tarsal tunnel syndrome
The treatment of tarsal tunnel syndrome should be geared to the underlying cause of the disease (varicose veins, benign tumors, fracture sequelae). If we suspect tenosynovitis or a local inflammatory process will use anti-inflammatory drugs, local corticosteroid injections, physiotherapy and orthotics rest.
- Infiltration ecoguide tarsal tunnel. When cases of foot deformity associated with good results by reducing the tension created on the posterior tibial nerve are achieved.
These measures are resorted to surgery when they fail. Surgical release includes four gestures: opening of the flexor retinaculum without further closure, opening the fascia of the adductor of the big toe, exoneurolísis the posterior tibial nerve and its branches all the way and sweeping of the fibroadiposos walls of the medial calcaneal branch.
Described endoscopic minimally invasive techniques tunnel opening and ultrasound is allowing the development of ultra-minimally invasive techniques for cases where there is no obvious cause compression that is to be resected.
- Surgery ultra-minimally invasive ultrasound - guided tarsal tunnel. The results are better when there is an objective reason giving rise to the syndrome, which if idiopathic or posttraumatic. The results will be better the less time has elapsed.
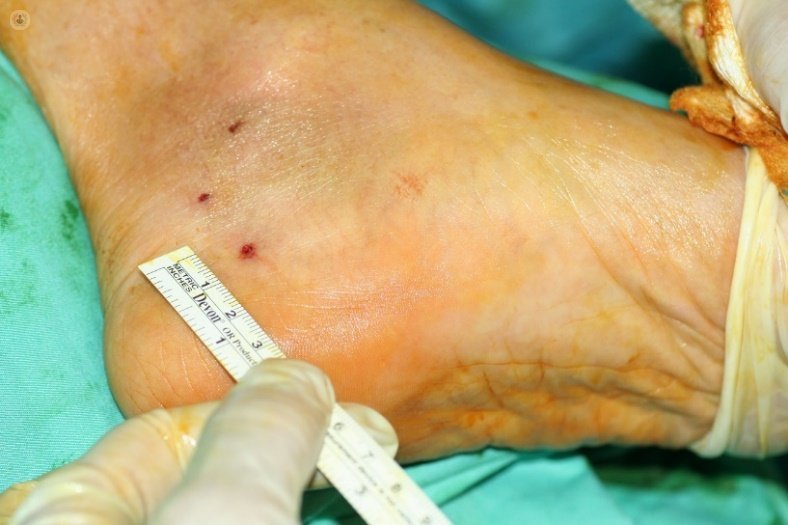
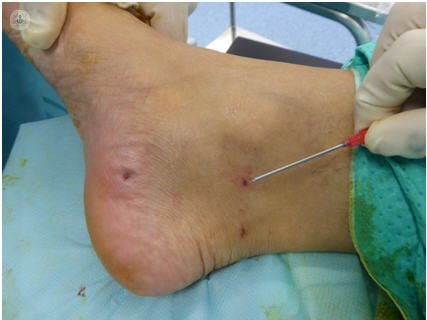
Rates published good results with conventional surgery vary between 50% and 90%. Recurrence of tarsal tunnel syndrome is difficult to treat and the results are less predictable. It usually occurs in older patients with long-standing compression, compression by a double level, inadequate surgical technique or the development of adhesions around the nerve.
In our opinion, the longitudinal incisions on the tarsal tunnel lot induce fibrosis, and the success rate is not very good.
If open surgery do we best make transverse incisions in the ankle calcaneus axis, and using magnifying glasses for release.
With ultramínimamente invasive surgery ecoguide are improving the results of open surgery and are added benefits, how to operate both feet at once, do not ischemia, not give points and a quick recovery, but its limitations are yet to be defined.


