Sleep bruxism: the importance of accurate diagnosis
Written by:Sleep bruxism is characterized by involuntary movements of the Masticatory Muscular Rhythmic Activity (ARMM). Some symptoms are: pain when feeling the masticatory musculature, dental wear associated with tooth grinding, pain of the temporomandibular joints or headache. The precise diagnosis and appropriate treatment are very useful, to rule out problems derived.
Bruxism of the dream: what is
Sleep bruxism is a sleep-related movement disorder characterized by the involuntary movements of Muscular Muscular Rhythmic Activity (ARMM) associated with micro-awakening phenomena and, occasionally, the presence of teeth grinding noises.
It is important to emphasize that for many years bruxism was considered a parafunctional masticatory activity, related to dental wear and pain in masticatory muscles. However, at present, the etiology of nighttime bruxism can be considered multifactorial.
In this regard, the greatest advance has been the recognition that the etiopathogenic mechanisms involved in bruxism of wakefulness (daytime tightening) and sleep bruxism appear to be completely different. This has caused a change in the diagnostic criteria, the design and orientation of the research studies and the therapeutic management of the same.
Prevalence of bruxism of sleep and bruxism of the vigil in society
Sleep bruxism is a frequent disorder, presenting an average prevalence of 8% in the general population. However, waking bruxism is characterized mainly by the presence of episodes of dental tightening rather than grinding, and tends to increase with age, with an estimated prevalence of 12% in children and up to 20% of the adult population.
It is important to note that sleep bruxism is often coexistent with waking sleep. Thus almost 1/3 of patients reporting sleep bruxism are also aware of the presence of this habit during wakefulness.
Signs and Symptoms of Sleep Bruxism
Patients who present with sleep bruxism usually report any of the following signs and symptoms:- hypertrophy (increase of volume) and pain on the palpation of the masticatory musculature (masseter and temporal)- indentations on the lateral edges of the tongue- presence of dental wear associated with tooth grinding.- preauricular pain at the level of the temporomandibular joints (TMJ)- presence of morning headaches
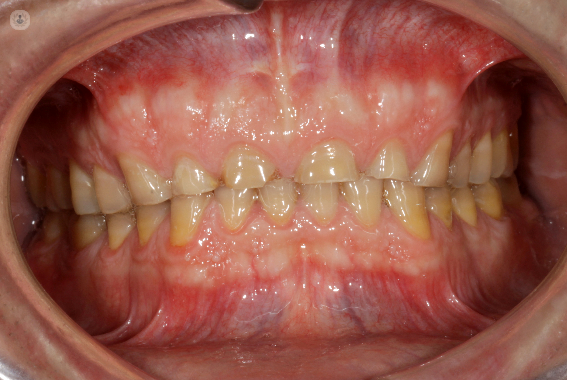

Diagnosis, therapy and treatment of sleep bruxism
In cases of sleep bruxism associated with morning pain in the masticatory musculature or when signs of dental overload (dental wear, tooth sensitivity, etc.), nocturnal use of a rigid occlusal full-arch splint may be indicated. control of the adverse effects of sleep bruxism on the masticatory apparatus. However, the grinding associated with sleep bruxism may persist even with the splint, since the patient continues to show progressive wear.


If there are other related risk factors such as OSAHS (Sleep Apnea-Hypopnea Syndrome), the use of Mandibular Feeding Devices (DAM) would be more appropriate.
In cases of sleep bruxism associated with anxiety, high levels of daytime stress or psychophysiological insomnia, in addition to cognitive-behavioral therapy, pharmacotherapy with anxiolytics (clonazepam) or beta-blockers (propanolol) may be indicated, always for short periods of time. Likewise, in those cases in which sleep bruxism is associated with daytime bruxism with significant contracture and hypertrophy of the temporal and masseter muscles, infiltration with botulinum toxin may be indicated.
In the bruxism of the vigil the patient usually attends the consultation of the expert in Dentistry and Stomatology , who will be in charge of its clinical management. However, the odontostomatologist who confronts a patient with bruxism of the vigil should not lose sight of two aspects:1) It is important to discard that the bruxism presented by the patient is a sign of an underlying disease or process (neurological, psychiatric illness, regular intake of medication or drugs, etc.). In such cases, it would be best to refer the appropriate specialist for its relevant treatment.2) There is a high degree of concordance between the presence of bruxism of the wake and sleep bruxism, the latter being also important for future diagnostic and therapeutic interventions. In this case, sleep-related respiratory disorders (OSAHS) are particularly important, given that, due to their high morbidity and mortality rates, they should be diagnosed as soon as possible.
Finally, it is important to note that the use of occlusal splints in a systematic way for the treatment of sleep bruxism should be questioned, since some of them, in certain situations, may aggravate the episodes of bruxism if there is a coexistence with respiratory disorders related to sleep. It is also important that the dentist who is in charge of the treatment has a specific training in Craniomandibular Dysfunction and Orofacial Pain, since these patients are often detected not only by the presence of dental wear but also by the presence of symptoms at the device level masticatory (musculature pain, arthralgia, headache, joint blockage of TMJs, etc.), which should be correctly diagnosed and treated.


