Learn how to identify and treat atopic dermatitis or eczema
Written by:Atopic dermatitis or eczema is a chronic and common disorder in which the skin is inflamed, red, dry and intense itching. It affects mainly children.
Atopic dermatitis is due to a combination of genetic and environmental factors. Genetic causes include differences in the proteins that form part of the skin barrier. When this barrier is broken the skin loses moisture and becomes dry, irritated and hypersensitive. Then skin shows a greater tendency to infection, either by bacteria, viruses or fungi. The immune system of the skin can vary and overreact to environmental factors , such as pet hair or dust particles triggers.
Notably asthma and allergies may occur more frequently in patients with atopic dermatitis, but they are not the cause of eczema.
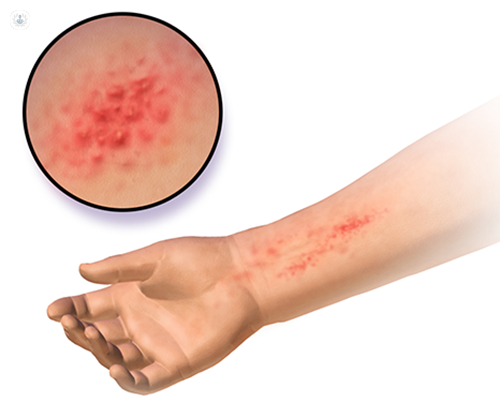
How and where atopic dermatitis affected by age
In young children, atopic dermatitis often begins as a dry red rash that affects the cheeks and around the mouth, worsening with pacifier use. As the child grows the eruption happens to affect the arms, legs and other areas where they can scratch. In teenagers, eczema affects mainly the inside of the elbows and knees, hands, feet and around the eyes.
Although there is no cure, usually it improves significantly with age and becomes disappear in a large proportion of patients. However, a number of recommendations to help manage this problem.
Treatment of atopic dermatitis
The treatments recommended by experts in dermatology for atopic dermatitis are aimed to prevent skin dryness, treat the rash, itching improve and minimize exposure to triggers. In this sense, the process to follow would be:
1) daily skin hydration to prevent dryness- A daily bath or every other day in order to keep the skin clean and remove potential irritants.- The water should be warm (not hot) and the bathroom should not exceed 5 to 10 minutes.- After the bath it is necessary to dry the skin thoroughly and apply moisturizer generously.- It is important to find a type of moisturizing cream or milk accept the child's skin because, otherwise, it will reject its application.- The thicker cream, better and better barrier function of the skin hydration.
2) Treat the rashThe most commonly used medications are topical corticosteroids. There are many types of them, with different potencies and formulations (ointments, creams, ointments, lotions, solutions, gels, emulsions, foams, etc.). In any case, the type of corticoid and its presentation will be adjusted to the individual patient, in order to get a good response and minimal side effects. In general, they are applied in a thin layer on the skin and without exceeding the two daily applications. Is exceptional observed undesirable effects of its application if we do as we recommend our expert doctor of Dermatology.
There is a new group of topical anti-inflammatory drugs that are very useful, especially in very thin skin areas such as the eyelids, armpits and English, where it is more appropriate to avoid topical corticosteroids.
For severe cases of atopic dermatitis or do not respond to the usual medication it may be necessary systemic medication. These drugs are somewhat more complex to use and require detailed tracking by dermatologist.
3) Treat itchingIt should be explained to the doctor if the child has very itchy or if it affects the quality of sleep. Oral antihistamines may help sleep, but fail completely calm itching and scratching.
4) Avoid triggersThe most common include excessive bathing without further hydration, low humidity, snuff smoke exposure, emotional stress, sweat, rubbing and skin exposure to products such as wool, soaps, fragrances and washing detergents.
5) Recognize infections as triggerAtopic children have impaired skin barrier and therefore have an increased risk of skin infections. The most common is infection by the bacterium Staphylococcus aureus, which should be suspected when the skin develops crusts with similar appearance dry honey. The infected skin can worsen eczema and some patients need topical and even oral antibiotics.
Edited by Patricia Crespo Pujante


